Illustration by Emma Günther
Perimenopause 101
Everything you need to know about when and why perimenopause happens, how long it lasts, and what changes to expect.
Top things to know about perimenopause
Perimenopause is the transition towards menopause (the point at which someone hasn’t had a period for 12 months or more).
On average, cycle changes start four to five years prior to menopause.
During perimenopause, levels of hormones like estrogen and progesterone fluctuate and then decline.
Daily habits, medications, and supplements may help with uncomfortable perimenopause changes.
What is perimenopause?
Perimenopause is the body’s transition towards menopause (‘peri’ comes from the Greek word for “around,” so the word literally means “around menopause”). While perimenopause has become more widely discussed recently, you may not have heard the term before because people often confuse it with menopause itself. Menopause is the point in time at which someone hasn’t had a period for a full year (1).
Perimenopause is a transitory phase that can be as short as a few months or last up to 11 years. On average, it lasts around four to five years (2-5). During perimenopause, reproductive hormones like estrogen and progesterone fluctuate significantly and then decline gradually, giving rise to new sensations, experiences, and changes (1,5). Perimenopause experiences differ widely across people and cultures. While every woman and person with a cycle will go through perimenopause, this important transitory time is still underrepresented in culture and research.
When does perimenopause start and end?
The exact start of perimenopause is hard to pinpoint precisely because it varies so much from person to person. One study found that changes in the predictability of menstrual cycles began on average between ages 47-48 in women transitioning towards menopause. But it can begin much earlier or later. In the same study, about one in three people who were still menstruating at age 45 reported unpredictable periods. At age 52, one in 10 people reported that they still had predictable cycles (2).
Menopause marks the end of perimenopause and happens on average at age 51, but most people reach it anywhere between ages 45-55 (2,4,6,7). About four in 10 women reach menopause by age 50, and nine in ten will reach it by age 55 (2).
Common perimenopause experiences
Perimenopause can be a transformative time in your life, as you go through several changes—physically, mentally, and emotionally (1,8). It’s normal that you may go through a mix of emotions during this time, ranging from feelings of positivity, empowerment, or indifference, to increased sensitivity, anxiety, or depression (8). Everyone’s experiences are unique, and knowing that all feelings (or lack of them) are valid is important. Tracking and sharing your experiences during this time can positively affect how you feel.
To understand when you might be entering perimenopause, it can be helpful to track any changes to your cycle and any experiences you notice. You can track perimenopause experiences in Clue and use custom tags to track further changes and details.
Typical experiences may include (1,9):
Hot flashes
Night sweats
Sleep problems
Changes to urination
Urinary tract infection
Changes in menstrual cycle length or period flow
Mood changes like low mood and irritability
Cognitive changes such as brain fog and forgetfulness
Everyone is unique, and no two people will notice the same perimenopause changes. Some people will have a lot of experiences and some may have little to none.
With Clue Plus, you can learn more about managing perimenopause experiences in our other articles in the Perimenopause section of the Clue Content tab. You can also keep track of your symptoms and experiences related to perimenopause and monitor changes over time.
How do I know what stage of perimenopause I’m in?
Perimenopause is divided into two stages: early perimenopause and late perimenopause. Early perimenopause typically starts when someone is in their mid-40s (10), but it can also start earlier or later. In early perimenopause, cycle length typically varies by around seven days or more (5). This increases as someone goes through perimenopause (5). The early perimenopause phase can last between one and eight years (5).
These cycle changes are caused by hormonal changes, specifically of estrogen and progesterone (5). At first, you may notice that your menstrual period arrives slightly earlier or later each cycle than you expect (5), and it may be lighter or heavier than before (1,11). Some common experiences include a change to the length of the cycle and longer or shorter periods (5,12).
In late perimenopause, it’s estimated that menopause is likely one to three years away (5). At this point, cycles can last about 60 days or more (5). As ovulation becomes less frequent, your period might go away for months at a time, and then return as you approach the later stages of perimenopause (5). Eventually, menopause is reached, and menstrual cycles come to an end, along with the period and the ability to become pregnant. About one in 10 people may stop menstruating more abruptly and experience a shorter phase of unpredictable cycles (2).
The diagram below shows an example of how your cycles may change during perimenopause (5).
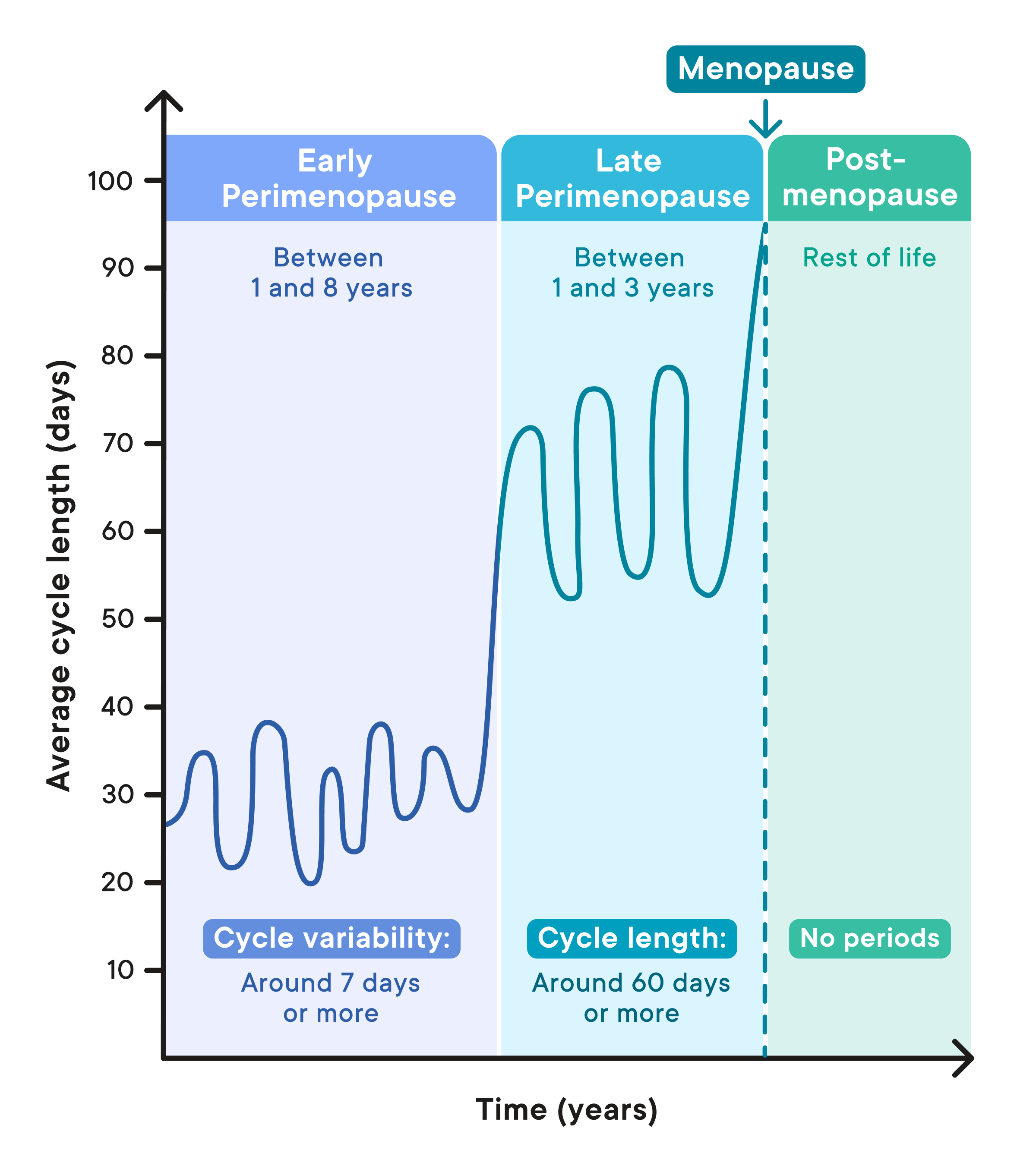
As your cycle changes, there may be times where you feel you’re waiting around for your next period. Understandably, this can be a stressful and worrying time for some women and people with cycles. It can feel like you’re not in control. It may be useful to track and compare your cycles and experiences to help you understand what stage of perimenopause you’re in. This can help you understand how far away menopause might be for you and provide support should you need to speak to your healthcare provider.
Navigating fertility changes
One of the better-known changes in perimenopause is the change in the chances of becoming pregnant during this time (13,14). You may begin to think more or less about your fertility and life choices. Tracking your experiences can help you feel empowered and support any decisions you might make about your care.
If you’re planning for pregnancy
If you’re seeking to become pregnant in perimenopause, it’s important to discuss your wishes with a healthcare provider. They can give you advice on whether you might require extra support or treatment. It’s recommended that anyone over the age of 40 be evaluated by an OB/GYN before trying to become pregnant (15).
If you’re avoiding pregnancy
While the risk of pregnancy is lower in perimenopause (14), you’ll still need to use a proven method of birth control diligently and consistently, as your cycle may be more variable and unpredictable (5). Many women opt for long-term options, like the IUD, during this time (14).
Reliable contraception should be used until menopause has been confirmed (14). Menopause can be confirmed by having no period for two years before the age of 50, having no period for one year after age 50, or by hormone testing by your specialist (14).
How do I manage perimenopause?
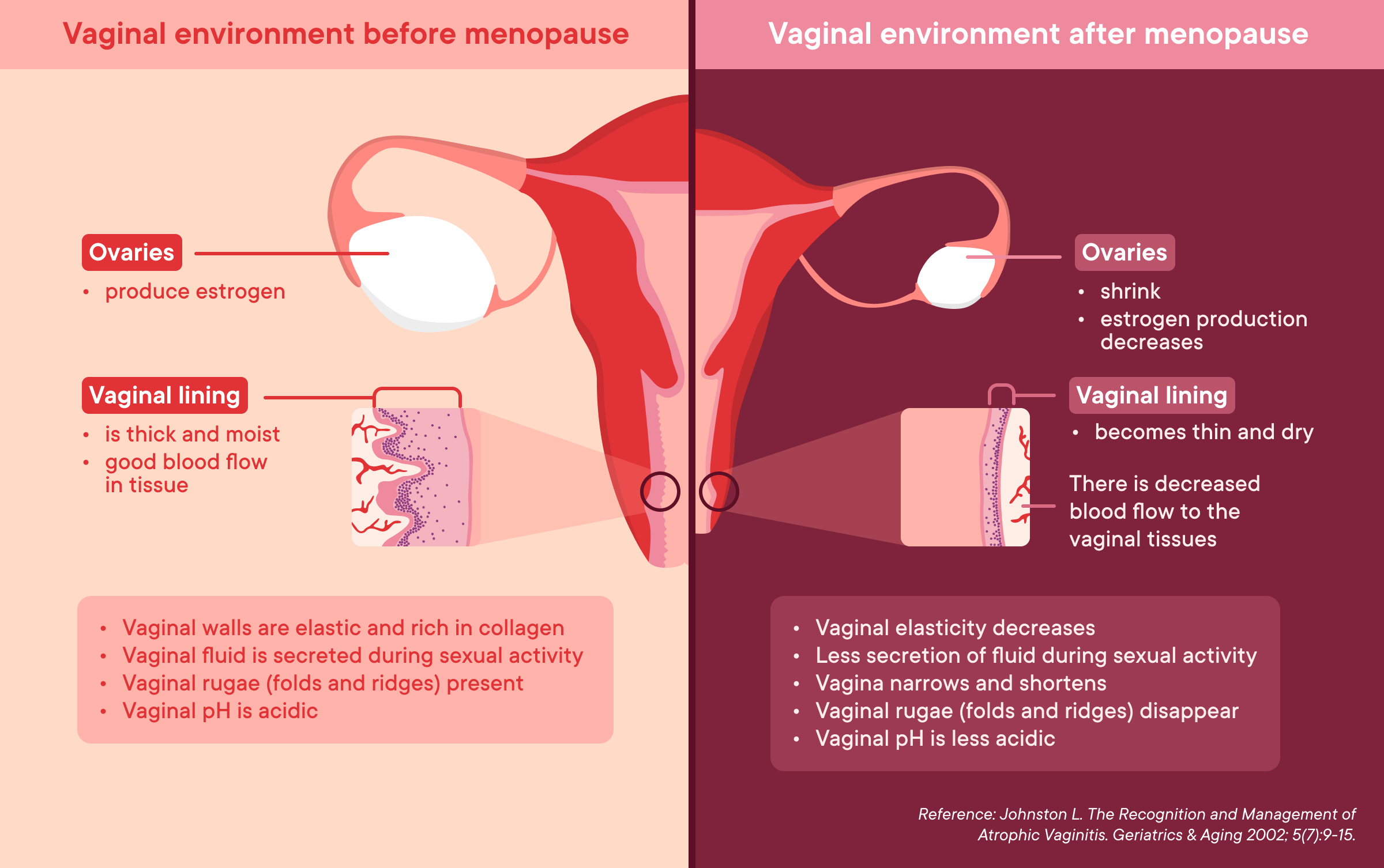
There are a number of simple tips you can work into your routine to help support your journey in perimenopause. Lifestyle changes such as regular exercise and stress management techniques like meditation can help with mood swings. Eating a balanced diet with enough calcium and Vitamin D can help to keep your bones strong while using products like vaginal lubricant will help with perimenopause symptoms like changes to the vaginal environment (vaginal dryness, thinner vaginal walls) (1,16). Sometimes hormone therapy such as menopausal hormonal therapy (MHT) (also known as HRT) or antidepressants such as selective serotonin uptake inhibitors (SSRIs) are prescribed during perimenopause to help relieve experiences associated with this time (17).
When to seek medical advice
Perimenopausal experiences can have a significant impact on someone’s quality of life. It may be a good time to check in with your healthcare provider if you have any concerns about your experiences, your changing periods, or if your everyday life or well-being is affected. Tracking and recording changes to your body and perimenopausal experiences in Clue can help you find the right treatment when visiting a healthcare provider.
FAQs
When does perimenopause start?
The start of perimenopause varies from person to person, but one study found that changes in the predictability of the menstrual cycle (a sign of perimenopause) began between ages 47-48 in women transitioning towards menopause. But it can begin much earlier or later. In the same study, at age 52, one in 10 people reported that they still had predictable cycles (2).
Can I still get pregnant during perimenopause?
While the chance of you getting pregnant is lower during perimenopause (14), you can still get pregnant. If you are trying to get pregnant and you are in perimenopause, you should speak to a healthcare provider to see if you need any further support. If you are trying to avoid pregnancy, you should use a proven method of contraception until menopause has been confirmed (14).
What are the most common signs of perimenopause?
Everyone’s experience of perimenopause is different. However, the most common symptoms of perimenopause include hot flashes, night sweats, sleep problems, vaginal dryness, changes in urination, urinary tract infections, changes in menstrual cycle length, period flow, or period volume, mood changes, and brain fog (1,9).
