Photography by Franz Grünewald. Art direction by Marta Pucci.
Ovulation pain: Symptoms, Causes and Treatment
What Does Ovulation Pain Feel Like?

Top things to know about ovulation pain:
About one in five women experience pain during ovulation that can last from a few minutes to 48 hours (1).
Ovulation pain is usually harmless, but can sometimes indicate a more serious medical condition like endometriosis (1).
See your healthcare provider if you are experiencing ovulation pain that is unusual for you.
What is ovulation?
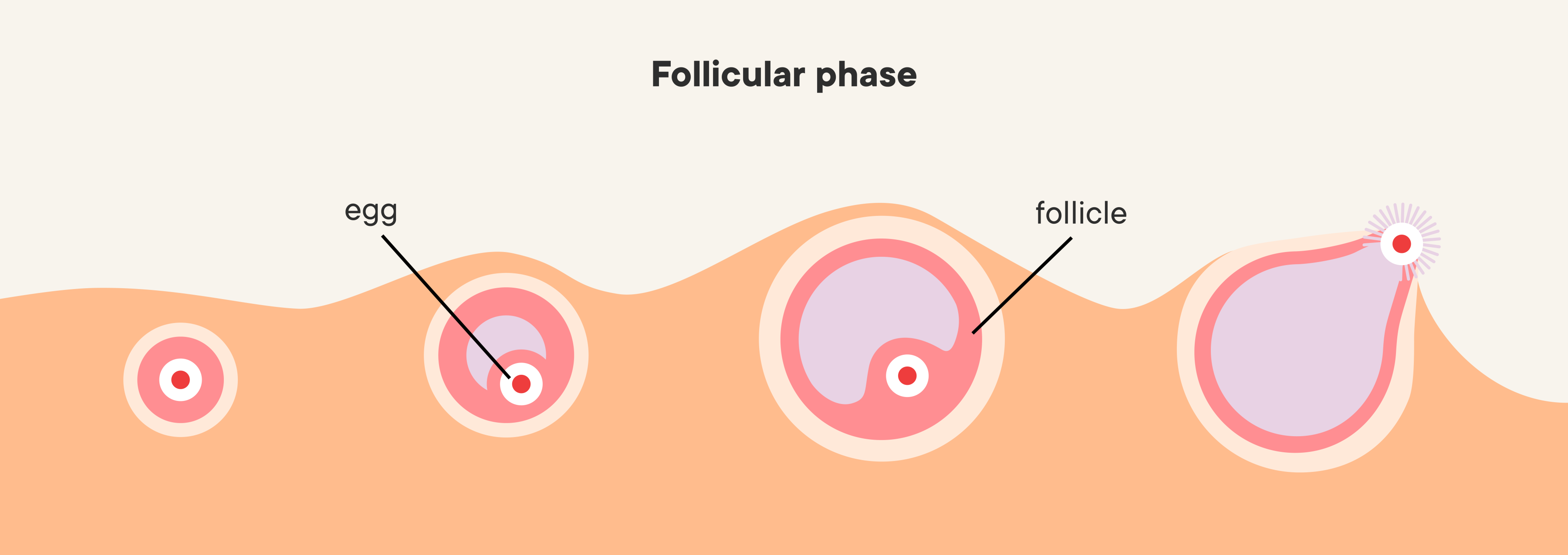
Ovulation is a major event of the menstrual cycle (2). During ovulation, your body releases an egg from a follicle in one of your two ovaries, which travels down your fallopian tubes to your uterus to prepare for possible fertilization (2). If the egg isn’t fertilized, the uterine lining (your endometrium lining) is shed during menstruation (3). If a sperm fertilizes the egg, it attaches to the uterus through a process called implantation (2). You are born with all the eggs you will ever have (4).

When does ovulation happen?
People have cycles with different lengths, so the timing of ovulation can vary from person to person (3). As an adult, you are probably ovulating in most of your cycles. If your cycle is within a 24-38 day range (which is considered “typical”) and your cycle doesn’t vary by any more than 7-9 days cycle-to-cycle, the chances are high that you are ovulating during your cycle. This usually applies to a menstrual period of up to 8 days (5). Cycles outside of those ranges can be an indication of anovulation and a reason to talk to your healthcare provider.
People with cycles usually report ovulation happening about 14 days before their period starts (6). This is not true for every person and every cycle (7). When you ovulate can vary based on the length of your menstrual cycle (7). If your cycle is between 27–34 days long, you may start to ovulate between days 13–20 (7). Some medications or medical conditions may stop ovulation or make it irregular (7).
Hormonal birth control, like birth control pills, can stop ovulation by increasing progesterone levels (8). Increased progesterone lowers the level of luteinizing hormone (LH), which in turn, inhibits ovulation (6).
Similar to most hormonal contraceptives, pregnancy pauses ovulation (9). After you give birth, it may take some time for ovulation to return, especially if you are exclusively breastfeeding (9).
When you reach menopause, you will stop ovulation completely (4). You are born with all the eggs you will ever have, and every time you ovulate, the overall number of eggs in your body decreases (4). With time, there will be no eggs left in your body for ovulation to occur (4). When this happens, ovulation will stop (4).
Some conditions will cause ovulation to be irregular. Polycystic ovarian syndrome, or PCOS, is the most common cause of long-term, irregular ovulation (4). PCOS may cause irregular menstrual cycles or cycles without ovulation, due to excessive androgen hormones and low estrogen levels (4).
Clue's research has found that in the last six months, 10% of Clue users tracked ovulation pain at least once.
What does ovulation pain feel like?
Ovulation pain typically begins a few years after a person starts menstruating (1). Do you ever experience an ache or sharp pain on one side of your lower abdomen near the middle of your menstrual cycle? Many of those who experience ovulation pain feel only a mild or dull ache that is short-lived (1). Some people describe ovulation pain as severe pain (1). One in five women experience discomfort during ovulation (1). If you have ovulation pain or mittelschmerz, you usually feel it every cycle. Ovulation pain can feel a bit like cramps.
Mittelschmerz appears between days 7–24 of your menstrual cycle and it usually goes away within 3–12 hours, but it can last up to 48 hours (1). Some people feel uncomfortable for a few minutes and others for a day or two (1).
Ovulation pain is felt on the same side as the ovary that is releasing an ovum (immature, unfertilized egg) (1). Typically, your left and right ovaries take turns ovulating every month (6). Your pain may switch location month to month depending on what ovary is ovulating (1).
What causes ovulation pain?
It’s important to note that research in this area is very limited. Ovulation pain most likely happens when the chemical hormone LH increases quickly in the body (1). LH is the hormone that causes a follicle (fluid-filled sac) in the ovary to release an ovum (6). This quick surge causes muscles in or near the ovary to tighten (1). LH surges about 36 hours before ovulation, and this is when you may experience ovulation pain (8).
Tracking with the Clue app can help you distinguish any patterns to discuss with your healthcare provider.
How can you manage ovulation pain?
There are no official treatment recommendations for ovulation pain. For most people, the midcycle pain resolves by itself and doesn’t require any treatment (1). Others may want to manage the pain the same way they would period cramps. Direct heat like a hot water bottle, a hot bath, or over-the-counter pain medications, such as nonsteroidal anti-inflammatories like ibuprofen or naproxen, may relieve pain (10). If the pain is bothering you, you can also rest until you feel better. Some people may benefit from using oral hormonal birth control pills from their OB/GYN to stop ovulation pain (1).
How to track ovulation pain with your cycle
Tracking when, where, how long, and the severity of the pain you feel around ovulation, can help you watch out for any medical conditions and possibly predict ovulation. You can bring this information to your healthcare provider to discuss possible treatment.
Track whether you feel it on the left side, right side, or both
Ovulation pain is typically felt on the side of the ovary that is releasing an egg that cycle. You can use custom tags or write personal notes in the Clue App. The pain may not be present every month, so tracking helps you keep a record and notice any patterns.
Track how long it occurs
Ovulation pain can last for a few minutes up to a couple of days (1). Clue has found that the majority of people who track ovulation pain do so for only one day. Others track it for two or more days. It is difficult to know to what extent other factors play a role, such as ovulatory pain due to endometriosis (11).
Track the sensation or severity
The sensations or pain of ovulation are as unique as the person who experiences it. For some, it’s not painful, just uncomfortable—some have described it as a mild ache (1). For others, it’s been described as cramp-like and sharp. It can be a mild pain for some people and a more acute and severe pain for others (1).
You can create custom tags in Clue to track any details of your ovulation pain. By tracking, you will have a better record of your experience, should you reach out to a healthcare provider.
Can ovulation pain help predict the timing of ovulation?
Statistically, the timing of ovulation pain tracked in Clue seems to be fairly promising as a predictor of ovulation.
However, ovulation pain is not a reliable way of predicting ovulation, as it can also be mistaken for other kinds of pain. Because of this, ovulation pain should not be used to prevent pregnancy or as the only method when trying to conceive.
Ovulation prediction tests/kits detect LH surges through urine tests and can track ovulation with an accuracy of up to 95% (8).
What conditions might be mistaken for ovulation pain?
Most ovulation pain is harmless and will subside on its own, but severe pain could indicate a health condition.
An appendicitis, ectopic pregnancy, or complications/ruptures of an ovarian cyst can all have similar symptoms as ovulation pain but tend to be more severe and unexpected (1, 12, 11). These conditions require immediate medical treatment.
Ongoing pelvic pain can be a sign of a health condition or infection such as sexually transmitted infections, inflammatory bowel disease, or endometriosis, which also require treatment or management from a healthcare provider (13,14,15,16). Scar tissue from c-sections or other abdominal surgeries can also cause similar pain on the side of your lower abdomen (1).
When should I see a doctor about ovulation pain?
You should seek medical attention if you have sudden, severe pain that isn’t going away with pain medication or pain that’s consistently getting worse (1). Tracking your ovulation pain with the Clue app can help guide your conversation with your healthcare provider or OB/GYN. You don’t need to live in constant or recurring pain that gets in the way of your daily life.
FAQs
How do you relieve ovulation pain?
You can use a hot bath or over-the-counter pain medication, like naproxen or ibuprofen, to relieve ovulation pain (9).
How long after ovulation pain is the egg released?
The egg is released from the ovary about 36 hours after ovulation pain. (8). Ovulation pain should not be used to predict ovulation.
Do ovulation pains get worse with age?
There is limited research in this area. Ovulation stops after menopause (9).
Does pain with ovulation mean I have a higher chance of getting pregnant?
All bodies are different, and there is limited research on whether pain with ovulation is a sign of increased fertility.
An earlier version of this article was published May 23, 2019.
