Art by Marta Pucci, photography by Franz Grünewald
What you need to know about ectopic pregnancy
Treatment and recovery from an ectopic pregnancy
Top things to know:
Ectopic pregnancies are not very common; only 2% of pregnancies are ectopic
An ectopic pregnancy occurs when an embryo grows somewhere in the body other than the uterus
You can become pregnant again after an ectopic pregnancy, depending on the treatment you received
Having one ectopic pregnancy doesn’t mean you’ll definitely have another one
An ectopic pregnancy is any pregnancy that doesn’t grow inside the uterus (1). There are some risk factors for an ectopic pregnancy — like if you’ve had surgery or an infection that affected your fallopian tubes (2, 3). Common signs of an ectopic pregnancy are vaginal bleeding and abdominal pain (3). Unfortunately, it is unlikely that an ectopic pregnancy can be saved. Depending on the type of treatment you need, it’s possible to become pregnant again.

At your first prenatal appointment, your healthcare provider may perform an ultrasound to see if the embryo is growing in your uterus. If it is growing outside of the uterus, you’ll need to talk about your treatment options. An ectopic pregnancy has serious risks to the pregnant woman or person and can be life-threatening. If you have been diagnosed with an ectopic pregnancy, we are here to explain why it happened, some options you can consider with your healthcare provider, and how to take care of your body and mind throughout the experience.
Why does an ectopic pregnancy happen?
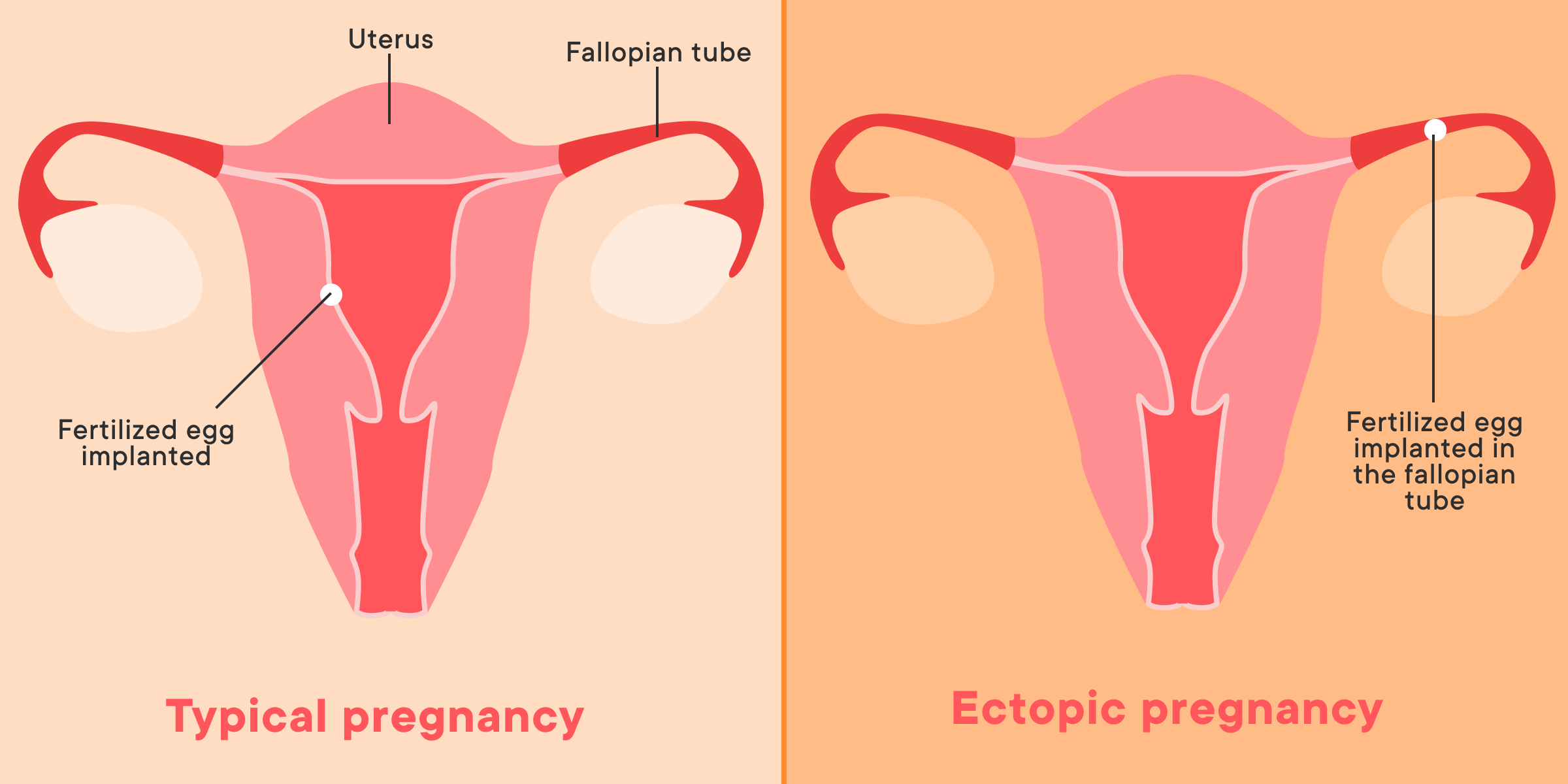
An ectopic pregnancy can happen when the fertilized egg doesn't make it into the uterus as expected (3, 10). Over 90% of ectopic pregnancies are in the fallopian tubes, where fertilization occurs (1). Ectopic pregnancies can also occur in other places in the body. An ectopic pregnancy can grow in the ovary, cervix, and even in scar tissue in the uterus that is there from previous surgeries (1).
Anything that can cause damage to the fallopian tubes like infections or surgery can put you more at risk for a tubal ectopic pregnancy (2, 3). Sexually transmitted infections like chlamydia, pelvic inflammatory disease, prior tubal or pelvic surgery, and endometriosis all increase the risk of ectopic pregnancy (3). Sometimes ectopic pregnancy can happen when you don’t have any risk factors, and there isn’t a clear explanation.
How will I know if I have an ectopic pregnancy?
It is difficult to diagnose an ectopic pregnancy without a healthcare provider and some tests. Ectopic pregnancies often seem like typical pregnancies. A missed period and signs of pregnancy like tender breasts or nausea are common (2).
Most people with an ectopic pregnancy will have some light vaginal bleeding or spotting (3). Abdominal pain and cramping on one side of the abdomen can be symptoms of an ectopic pregnancy (2). It’s also possible to have an ectopic pregnancy without any vaginal bleeding or pain (3).
So, how can you know if you have an ectopic pregnancy? Some healthcare providers recommend an early first-trimester ultrasound to see where the pregnancy is located (1). If you are pregnant, talk to your healthcare provider to see if this is right for you.
If you are pregnant and have any vaginal bleeding with abdominal pain, check with your healthcare provider as soon as possible. They need to determine if your pregnancy is ectopic, if something else is going on, or if your experiences are typical during the first trimester (2). If the pregnancy is ectopic, an ultrasound, blood tests, and a check-up will help your healthcare provider decide which treatments to offer you (1).
Ectopic pregnancies need treatment because as a tubal ectopic pregnancy grows, there is a risk of rupture in the fallopian tube. This is called a ruptured ectopic, and is a life-threatening emergency. If you are pregnant or could be pregnant and experience sudden abdominal pain, shoulder pain, or weakness, these can be symptoms of a rupture and you should seek healthcare immediately (2).
Can an ectopic pregnancy be saved?
It is extremely unlikely that an ectopic pregnancy can be saved. Any ectopic pregnancy in the fallopian tubes does not have enough room to grow. If left without treatment, it will eventually cause that tube to rupture — a medical emergency (2). No matter where the pregnancy grows, if it is outside the uterus, it cannot be saved without causing serious risk to you (3).
What are the options for handling an ectopic pregnancy?
It is important to receive treatment for an ectopic pregnancy. An ectopic pregnancy that continues to grow can be very dangerous to the mother or pregnant parent and even be life-threatening (1).
Option 1: Medication for ectopic pregnancy
If the ectopic pregnancy is found early enough, a common treatment option is a medication called methotrexate. Methotrexate works by stopping cells from growing, which stops the pregnancy (2). Methotrexate isn't the right treatment for everyone. It is not recommended for people with kidney or liver disease or if you are breastfeeding/chest feeding (1, 2).
This option will require visiting your healthcare provider a few times to make sure the medication is working as expected (1). Your healthcare provider will test your pregnancy hormone levels with a blood test until they are negative, indicating that you are no longer pregnant (2).
Methotrexate is typically given as an injection in your muscle and you may need several doses (1, 3). Side effects of methotrexate can include nausea, vomiting, diarrhea and abdominal pain (2). These side effects are not as serious as the side effects of untreated ectopic pregnancy.
Option 2: Surgical treatment for ectopic pregnancy
Your healthcare provider will probably recommend surgery for ectopic pregnancy if you have intense pain or are showing signs of a ruptured tubal pregnancy (1, 2). Surgery is also recommended if there are other medical reasons you shouldn't take methotrexate or if the methotrexate doesn't work (1).
Unless emergency surgery is required, a laparoscopic surgery is typically performed to remove the pregnancy from the tubes or wherever the pregnancy is located (2, 3). A laparoscopic surgery uses very small incisions with the help of a camera. There is typically less pain, risk of infection, and time needed for healing compared to traditional surgery (1, 2).
Your healthcare provider should discuss the surgical options with you. The options are usually a salpingostomy or salpingectomy depending on how much damage there is to the fallopian tube and your plans for becoming pregnant in the future (1). A salpingostomy creates an opening in the tube to remove tissue (3). A salpingectomy is the removal of the tube (3). If you desire pregnancy in the future, your provider will likely attempt to keep your tube if possible (1).
Option 3: Watch and wait
Your healthcare provider will most likely recommend either medication or surgery if you have an ectopic pregnancy. If your tubal pregnancy is found very early and you have very low levels of pregnancy hormones that are already decreasing on their own, you may not need medication or surgery (3). Even if you don’t need medication or surgery, it is still very important to your safety to continue to visit your healthcare provider and follow their plan.
Becoming pregnant again after an ectopic pregnancy
After an ectopic pregnancy, some people want to wait to get pregnant again. If you want to prevent pregnancy you can start any form of birth control (6). Check with your healthcare provider to see what might be best for you.
The return of your cycle, and when you can try to conceive again, will depend on how you treated the ectopic pregnancy. Each person's recovery may be slightly different, but for most people, it takes a few cycles before your period returns to your version of normal (2).
If your ectopic pregnancy didn’t need treatment, you can try for pregnancy when a healthcare provider has confirmed that the ectopic pregnancy is no longer present, and you feel emotionally and physically ready (1, 2).
If you took methotrexate to resolve the pregnancy, it is recommended to wait 12 weeks (the time it takes for the medicine to be completely processed by your body) before trying to conceive (1). This is because medicine could impact the development of an embryo in a new pregnancy (1).
If you had surgery to remove the ectopic pregnancy, your ability to become pregnant again will depend on a few things. Removal of the fallopian tube and scarring from the surgery can reduce your chances of becoming pregnant in the future (5). Talk to your healthcare provider about your specific situation to find out how becoming pregnant again might work for you.
Sometimes there is damage to the tissue where the ectopic pregnancy occurred. People who have had an ectopic pregnancy once have a 10% risk of having another (1, 5). This does not mean that you have a higher risk for other types of miscarriages in future pregnancies (4).
Taking care of your mental health
While most of the support you’ll receive for an ectopic pregnancy helps you recover physically, know that your mental recovery is just as important. If you have a life-threatening experience or the ectopic pregnancy impacts your ability to become pregnant again in the future, know that you may be at risk for post-traumatic stress disorder (PTSD), anxiety, or depression (7).
Ectopic pregnancy can be a hard experience, no matter what the outcome. You may have a wide range of feelings after an ectopic pregnancy. Emotions after a pregnancy loss are complicated and differ for every person. You may feel grief and this grief is real. But it is also okay if you feel something different or don’t have many feelings about it at all.
It is important to give yourself time and seek support if you need it (2). Counseling has been shown to help the grief process (8). Talking about your feelings and receiving support from friends and family can decrease symptoms of grief, depression, and anxiety (8).
If you experienced ectopic pregnancy, we are sorry. Whether the pregnancy was planned or not, an unexpected outcome like this one can be trying both physically and emotionally. Here is a list of online resources and books below that may be helpful as you recover.
Resources
Online resources:
Books to read:
How to Carry What Can’t Be Fixed: A Journal for Grief — by Megan Devine
Surviving Pregnancy Loss: A complete sourcebook for women and their families — by Rochelle Friedman and Bonnie Gradstein
Virtual therapy:

