Illustrations by Emma Günther & Marta Pucci
Going off of birth control
Myths, misconceptions, and the time it takes to conceive when stopping birth control
Top things to know about going off birth control:
Hormonal birth control prevent pregnancy by stopping ovulation
You do not need to detox from birth control
Most people will become pregnant within a year when trying to conceive
There is a common misconception that using birth control may make it harder to become pregnant in the future (1, 2, 3).
Hormonal methods of birth control prevent pregnancy by stopping the body from ovulating (the release of an egg) (4). After the method is removed or stopped, ovulation usually returns along with the chance of pregnancy (4).
How much time will it take to become pregnant after stopping birth control?
Many people will conceive in just a few months after going off birth control (1, 4, 5).
The time it takes for birth control to leave the body depends on what it is made of, and how it is put in the body (4). Some methods take longer to leave the body than others (we’ve broken down each method below).
In general, 84-90% of people trying to conceive will become pregnant within one year of not using birth control and having sex 2-3 times a week—whether they have recently ended birth control or not (4,6,7). This is true for all birth control methods (1, 4, 8).
Your body does not need to detox from birth control
There is nothing you can do to help birth control leave the body. The body will remove medications, including hormones from birth control, on its own.
When ovulation returns, pregnancy becomes possible again (4). If you become pregnant immediately after stopping your birth control method, there is nothing to worry about (9). Research shows that hormones from birth control do not cause harm to a developing fetus (9).
Conceiving is also not affected if you skipped “periods” (withdrawal bleeds) while using a birth control method (4).
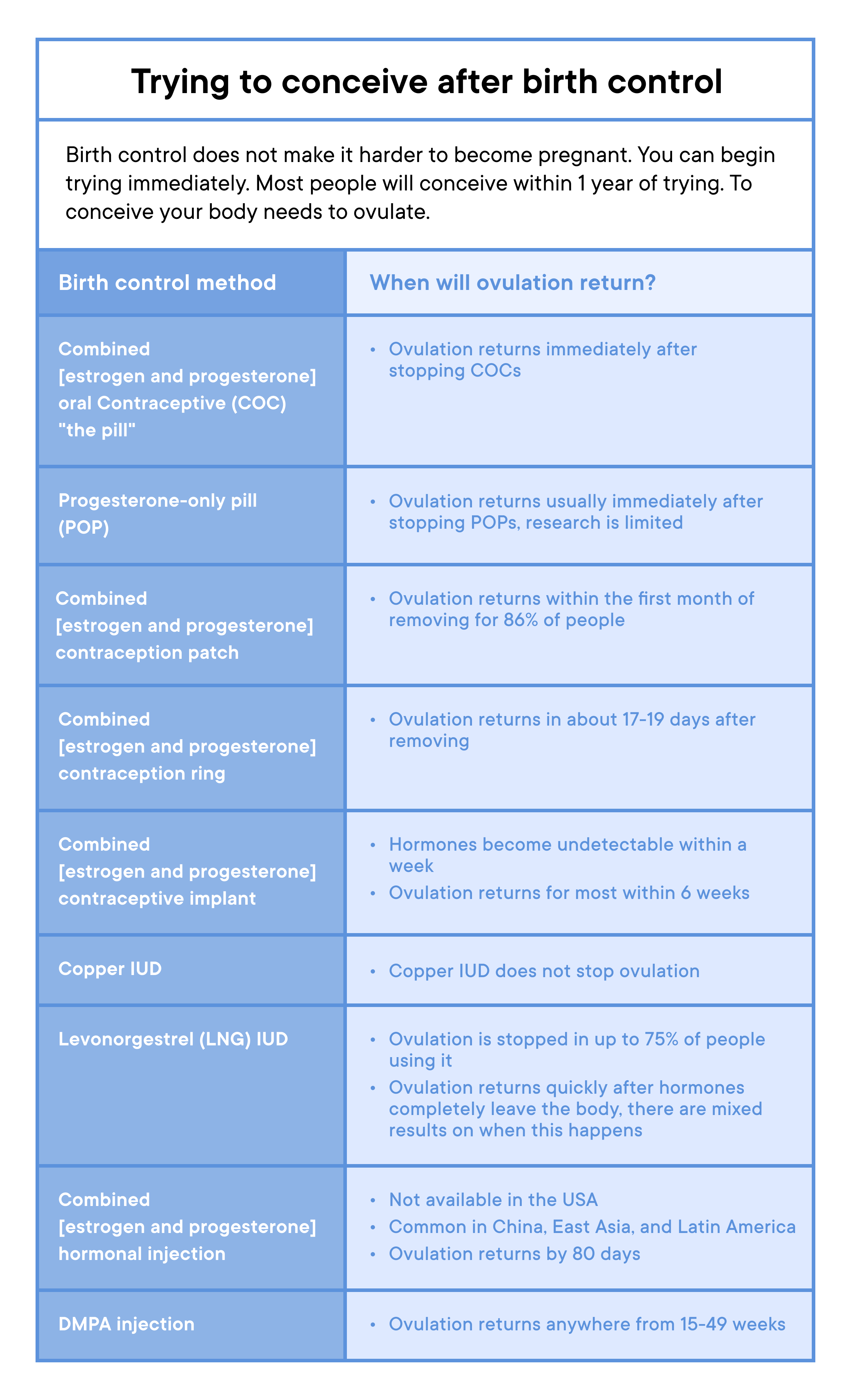
How long do the hormones from each birth control method take to leave the body?
If you want to conceive after ending birth control, you can begin trying immediately. There is no benefit to waiting based on birth control.
Your body needs to ovulate to become pregnant (4). Depending on the method you are ending, the time it takes to start ovulating may differ (4).
Combined contraceptives
Combined contraceptives contain synthetic versions of two hormones: estrogen and progesterone (4). They are called ethinyl estradiol (EE) and progestin (4).
The pill (ethinyl estradiol (EE) & progestin)
Natural menstrual cycles and ovulation often begin immediately after stopping combined oral contraceptives (COCs), but it may take some months for your period to return (10).
The pill was first available about 65 years ago and contained much more ethinyl estradiol (EE) than modern versions (4, 11). Because previous versions had such high amounts of hormones, it may have taken longer to exit the body. This may be where some people's worry around birth control and conceiving originated.
Because of the smaller amounts of EE currently used, periods now return quickly after ending COCs (4, 10). One study showed that most people saw their period return within the first 3 months after they stopped taking the pill (10).
The patch (ethinyl estradiol (EE) & progestin)
For 86% of people, ovulation returns within the first month after they stop using the patch (4).
The ring (ethinyl estradiol (EE) & progestin)
Ovulation is estimated to return about 17-19 days after removing the ring (4).
Progestin-only Contraceptives
Progestin-only contraceptives contain the synthetic version of the hormone progesterone.
The “mini-pill” (progestin)
Ovulation usually returns immediately after stopping progestin-only pills, but there is limited data on this method (4).
The implant (progestin-only)
The hormones from the implant become undetectable within a week of removal (4). Ovulation returns for most within six weeks (4).
The hormonal IUD (Levonorgestrel [LNG] IUD)
There are several different types of IUDs with different amounts of the progestin levonorgestrel (4, 12). For all types, ovulation may stop during the first year after the IUD is placed, but does not always stop (12).
Ovulation returns in almost all cycles by the time the IUD is supposed to be removed (12). If ovulation is not already happening, ovulation should return quickly after the IUD is removed (1,4). You can start trying to conceive as soon as the IUD is removed (4). The rate of conceiving within one year after using a hormonal IUD is the same as people using no birth control at all (1).
The birth control shot
The injectable birth control method Depo-Provera (medroxyprogesterone acetate [DMPA]), has a chance of causing a delay when trying to conceive (4). This is because the birth control is injected into the muscle and is used slowly by the body (4, 13). It can take up to 12 weeks for DMPA to completely leave the body (14, 15).
Studies show ovulation may return anywhere from 15-49 weeks after your last shot, and that it may take up to 9-10 months to conceive (4, 5). This is a large range and makes guessing how long it will take to become pregnant difficult (4). Tracking your cycle and signs of ovulation can be helpful in identifying ovulation and timing sex.
The copper IUD
The copper IUD does not contain synthetic estrogen or progesterone (4). Instead, the copper in the IUD causes chemical reactions in the body that make it hard for sperm to move, and the T-shaped device changes the environment in the uterus (4).
Pregnancy can happen within the first month of removing a copper IUD, and studies show that more than half of all people trying to conceive become pregnant within six months and up to 97% become pregnant within a year (1).
What affects the time it takes to get pregnant?
Age, reproductive and general health conditions, nutrition, and timing of sex, among other factors, all have the potential to impact the time it takes to conceive. This is true for anyone, no matter how long, or if they have ever, used a birth control method (6).
Anything that affects how often your body releases an egg, the genetic makeup of the egg, or the ability of egg and sperm connecting can impact the chance of conceiving (16). Monitoring your cycle and ovulation experiences in the app can help you determine the best time to have sex to conceive (16).
Assisted reproductive technology (ART)
For many reasons, some people that are trying to conceive will need to use assisted reproductive technology (ART). ART means that egg and/or sperm are handled in some way by a healthcare provider during the process of becoming pregnant (6). This can include ovulation induction (OI), intrauterine insemination (IUI), In vitro fertilization (IVF), and surrogacy, among others (6). Talking with a fertility specialist can help you understand the best treatment options for you (6). The American Society for Reproductive Medicine is a good resource for learning about ART in the USA.
When should I see a healthcare provider?
Consider consulting your healthcare provider if:
You have ended your birth control method and have not had a period for 3 months (17) There may be other reasons why your cycle has not returned, such as PCOS, that were hidden while on birth control (6)
You are 34 or younger, having regular sex (2-3 times a week) for 12 months, and have not become pregnant (18)
You are 35 or older, and have not become pregnant after 6 months of frequent sex (18)
You are over 40 It is recommended that you talk with an OB/GYN before trying to conceive (19)
All of this said: try not to get hung up on numbers or the likelihood of conception. Trust your body. If you feel like becoming pregnant is taking longer than it should, reach out to your healthcare provider for additional guidance and reassurance.

