Illustration by Katrin Friedmann
The immune system and the menstrual cycle
Your immune system is the basis of your health. Most of the time, it works for you by fighting off infection and helping fix injury. Although sometimes your immune system works against you, causing or influencing chronic diseases like allergies and arthritis.
Sex hormones, such as estrogen, progesterone, and testosterone, seem to affect the immune system and its function. There is evidence to suggest that premenopausal people’s bodies react differently to illnesses and infections over the course of their menstrual cycle due, at least in part, to fluctuations in sex hormones.
Understanding how your immune system functions can help you appreciate and anticipate your healthy days and less-healthy days.
Your immune system can be roughly broken into three categories:
- Innate immunity: This includes secretion of mucus and some types of immune cells.
- Inflammation: When your body is exposed to foreign substances, such as bacteria, or are injured, your immune system will stage an inflammatory response. Acute inflammation helps protect tissue and increases the number of immune cells at an infection or wound site, while chronic inflammation can lead to chronic diseases.
- Acquired immunity: We develop acquired immunity when exposed to bacteria, viruses, and other substances. Acquired immunity includes B and T lymphocytes, and antibodies that have developed in response to infection and vaccination (1-3).
The first part of your cycle: the follicular phase
During the follicular phase of the menstrual cycle (i.e. the first part of the cycle, from the first day of the period until ovulation), people tend to have higher levels of antibodies in their body and have an increased inflammatory response (1, 4). These changes makes people less susceptible to infection during this phase of their cycle (1, 4).
This increased immune response is thought to be partially triggered by rising estrogen levels that occur between menstruation until just before ovulation (1, 5, 6). Estrogen interacts with immune cells by attaching to receptors on the outside of the cells, and by interacting with cell processes occuring in the nucleus and cytoplasm (4, 7). During the follicular phase, this interaction increases inflammation, though estrogen doesn’t always necessarily have that effect (1).
Higher estrogen does not necessarily mean better health, as the higher inflammatory response caused by estrogen can lead to a worsening of chronic disease (1, 4, 7). Also, prolonged exposure to endogenous (i.e. from the body) estrogen is associated with the development of certain cancers, such as breast cancer (8).
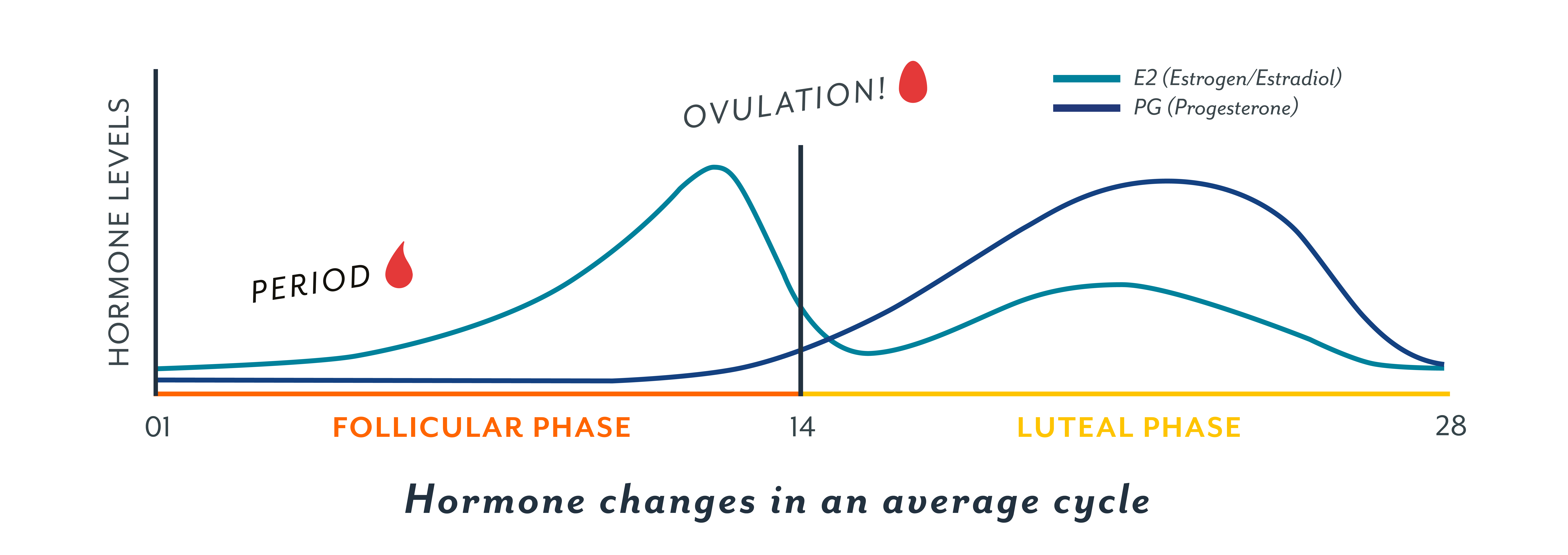
The middle of your cycle: the early and mid-luteal phase
Conversely, during most of the luteal phase of the cycle (i.e. the second part of the cycle), the immune system is suppressed and much less likely to stage an inflammatory response (1, 4). This suppression of the immune system during the luteal phase is associated with rising levels of progesterone and with cellular changes that influence testosterone (1, 4-6, 9). These effects from progesterone and testosterone could be considered positive or negative, depending on the disease.
On one hand, many people experience fewer symptoms from chronic diseases, such as asthma, during the early and mid-luteal phase (1, 4).
Inflammation can worsen symptoms of many chronic diseases, and so this suppression of inflammation can be a good thing.
On the other hand, although inflammation has a bad reputation, having a suppressed inflammatory response increases a person’s risk of infection (1, 4). This decrease in inflammatory response might be one reason people with cycles have reduced ability to build muscle during the second half of the cycle, but more research is needed (10, 11).
How testosterone affects the immune system is a little less clear. Interestingly, the effects of testosterone might vary not only in response to progesterone and estrogen, but also potentially in response to sexual activity (5, 9). More research is needed to understand how the effects of testosterone on the immune system are mediated by hormones and behaviors.
The last part of your cycle: the late luteal phase and menstruation
In the few days preceding and throughout menstruation, people are more likely to experience negative or worsening of symptoms from chronic health conditions, such as asthma or arthritis, as their inflammatory responses return and as levels of a hormone-acting lipid called prostaglandin increase (1, 4, 5, 12, 13). Although estrogen levels are low during this time, menstruation itself is associated with increased inflammation, though there is not a clear understanding of how or why (1).
Why does this happen?
In theory, your body functions this way to promote pregnancy (1). When people are in the early to mid-follicular phase of their cycle, they can’t get pregnant, as they haven’t ovulated yet (14).
During this time, your bodies want to fight off all foreign invaders so that you can stay healthy enough to become pregnant.
However, around ovulation (which is when estrogen levels drop-off) (6), your immune system is downregulated by progesterone in order to prevent immune cells from attacking a fertilized egg and from preventing implantation (1). Testosterone, depending on the phase, will encourage or suppress regulation of different immune cells (5, 9).
Although this theory feels intuitive, we don’t currently understand many of the biological mechanisms behind the menstrual cycle, pregnancy and menopause, and as such more research is needed to understand how the hormonal changes these stages of life present interact with the immune system (1, 4).
Hormonal birth control and the immune system
Hormonal birth control (HBC) always contains a synthetic progesterone (called progestin) and sometimes contains estrogen, depending on the type (15). HBC works by keeping the levels of sex hormones high, which prevents ovulation and/or thickens cervical mucus.
Current research suggests that HBC has both positive and negative effects for long-term health. Regarding short-term health, some evidence suggests that HBC, particularly progestin-only forms may create a reduced inflammatory state (like in the luteal phase) that increases the risk of infection (1, 15-17). However, this relationship is not well understood and currently there is no recommendation for those at high-risk of STIs to not use HBC (15).
Download Clue to track illness in the “Ailments” category.

